There are now various corneal refractive procedures available to correct vision, ranging from laser excimer to small lenticule incision surgery (SMILE). This article assesses the existing options and gives a glimpse into what the near future holds.
Trokel introduced the excimer laser in 1983 to treat refractive errors.1 The first photorefractive keratectomy (PRK) procedures were performed in Australia in 1991, followed by laser in situ keratomileusis (LASIK) in 1995. Since then, the available technologies have continued to evolve – the question now is which procedure is most appropriate for each patient?
analysis of a typical metropolitan refractive practice gives an insight into the demographics of patients who are seeking some form of surgical alternative to glasses and contact lenses
My colleagues and I assessed, over a 12 month period, 1,150 patients who presented wishing to have vision correction surgery.2 This analysis of a typical metropolitan refractive practice gives an insight into the demographics of patients who are seeking some form of surgical alternative to glasses and contact lenses.
The mean age of patients was 38, with a range of 18–79 years. Patients in the cataract population were interested in vision correction surgery. The mean preoperative spherical equivalent was -2.88 with a standard deviation of 3.41D, but with a range of -20.00D to +10.75D. The majority of patients were myopic, but with a very large range to the extremes of refractive error correction. The mean keratometry was 43.47 with a standard deviation of 1.61D, and a range of 36.85D to 61.50D. Patients with previous corneal laser turned up wanting something else done years later and patients with keratoconus were likewise seeking a surgical correction.

Figure 1. Tear osmolarity values
In this cohort, 37 per cent felt their eyes were dry when specifically asked and 22 per cent used artificial tears. Sixty per cent had an abnormal ocular surface disease index (OSDI) and at least one abnormal tear osmolarity score. Those with a disturbed ocular surface seek out refractive surgery for two reasons:
(1) They may be experiencing difficulties with contact lens wear,
(2) They may be having fluctuation in their vision because of their less than ideal tear quality.
These patients are under the care of optometrists and ophthalmologists, and my message is this: The general population needs to be better educated about the specifics of their ocular abnormalities, not just their refractive error, but also the quality of their tears. Dry eye disease is very common in the context of digital devices and prolonged near work.
When I reviewed my practice for the last 12 months, of those patients suitable for corneal laser surgery, 20 per cent received PRK, 30 per cent received LASIK and 50 per cent received SMILE. I’ll look at each of these procedures in turn.
PHOTOREFRACTIVE KERATECTOMY
The latest Cochrane review to compare LASIK and photorefractive keratectomy (PRK) was published in 2013.3 The conclusion was that LASIK gives a faster visual recovery and is a less painful technique than PRK, but with similar outcomes one year after surgery.
In the 1990s PRK led to unpredictable corneal haze and prolonged visual recovery and sometimes a drop in best corrected vision. In those early days of PRK, simply by increasing the optical zone and improving ablation profiles, the incidence of corneal haze reduced, but it was antiproliferative agents (topical mitomycin) that dramatically reduced the incidence of postoperative haze.4
The general population needs to be better educated about the specifics of their ocular abnormalities
Majmudar.P.A.5 et al reviewed the use of mitomycin-C (MMC) for the American Academy of Ophthalmology in 2015 and looked at its reported use over the previous 15 years. They found good evidence for the effectiveness of MMC when used intraoperatively as prophylaxis against haze in higher myopic ablations. However, they noted that the optimal dosage, effectiveness as prophylaxis in lower myopic and hyperopic ablations and long-term safety, particularly in eyes with reduced corneal endothelial cell counts from prior intraocular surgery, had yet to be established. Surface laser can be performed in a variety of ways. The most common is alcohol softening and manual removal of the epithelium and then direct ablation to the basement membrane, passing through Bowman’s layer and then the corneal stroma. More recently, transepithelial photorefractive keratectomy has become popular. Laser assisted subepithelial keratectomy (LASEK) and epipolos laser assisted in situ keratomileusis (EpiLASIK) are two surface procedures that are not commonly performed. All surface procedures seem to produce similar refractive results.6
I routinely use trans-epithelial PRK. It is as close to a no-touch procedure as it is possible to get. The ablation is performed directly onto the corneal epithelium.
The refractive ablation is performed first, then immediately following by a phototherapeutic keratectomy (PTK) ablation. I use mitomycin 0.02 per cent routinely in all patients via an 8mm soaked sponge. It is applied directly to the stromal bed immediately following the laser procedure and is left in place for a minimum of 20 seconds for any patient up to 3.00D spherical equivalent correction. Above 3.00D I add 10 seconds for every increased dioptre, up to a total of 60 seconds of application.
Immediately after the procedure, a bandage contact lens is applied. The lens is removed at day four post-operatively, by which stage the corneal epithelium is intact.
Trans-epithelial PRK appears to have some clinical advantages. The no-touch reduces the very low risk of infection to be even lower. Alcohol to soften the epithelium causes an inflammatory change and my clinical impression is that trans-epithelial PRK provides a slightly more comfortable post-operative course, with a slightly faster reepithelialisation and visual recovery. These are subtle but small improvements, and have made PRK a more viable procedure when compared to LASIK and SMILE in recent years.
PRK patients are generally able to return to work and driving one week after surgery, but it is sometimes two weeks and occasionally longer depending on epithelial remodelling, which is the limiting factor in the speed of recovery. Trans-epithelial PRK is generally not considered sensible in certain circumstances such as very low corrections (1.00D and below), or in patients with a corneal epithelium that may not be of a normal thickness. This includes previous corneal laser patients, where the corneal epithelium is variable in its thickness because the corneal shape has been altered. Similarly, in a post corneal transplant patient or a post radial keratotomy patient. Currently transepithelial PRK uses a standard assumption about the corneal epithelial thickness and it is assumed that the procedure would be even more effective if the corneal epithelium could be measured in each individual patient and the treatment tailored to them specifically.
PRK is generally the preferred procedure when the corneal anatomy is not considered ideal for SMILE or LASIK. My personal rule of thumb is that if the corneal thickness is below 500μm at any point, or if the Pentacam Belin/Ambrosio display has a combined score beyond 1.6, then I do not perform LASIK or SMILE. These are fairly strict criteria according to my preference, and I would not criticise those who perform SMILE or LASIK in a sub 500μm cornea.
In other circumstances, I would suggest PRK if LASIK has been performed many years previously and you do not wish to re-lift the LASIK flap because of the risk of epithelial ingrowth, or in a SMILE patient who requires an enhancement. PRK is a particularly good option in patients who have had cataract surgery where there is a small remaining error in one eye. PRK in this circumstance has minimal effect on dry eye because the treatments are often very small, and the speed of recovery is not critical given the other eye has not been operated on. This is a safe and effective way for the general ophthalmologist to perform an enhancement for residual refractive error following intraocular lens surgery.
In the past I would have selected PRK for patients returning to body contact sport, such as professional boxing or martial arts, however following the introduction of SMILE there is no longer an advantage in doing so. It has been suggested in the past that PRK has less effect on dry eye than LASIK. This has never been definitively proven. If the tear quality is borderline but the patient’s corneal anatomy is otherwise suitable, today I would suggest SMILE.
For the co-managing optometrist, the first few weeks of the postoperative period can be difficult as vision is still recovering and may be unstable through the day. Sensible expectations should be established prior to surgery – often the corneas of PRK patients are thin preoperatively and no further enhancement will be possible. Postoperatively, the patient needs to be reassured that their vision will recover – it simply takes time and cannot be hurried. Stromal and epithelial remodelling occurs for many months and the final visual result can take 12 months. Patients who are concerned at the one to two month mark can be reassured that their vision will continue to improve for many months. If an enhancement is required it should be delayed, in my view, for a minimum of 12 months after PRK to be certain of refractive stability.
It is very rare in 2019 to see significant corneal haze if topical mitomycin has been used. If it does occur it tends to peak at around three months, and if there is a drop in best corrected acuity it would be sensible to contact the ophthalmologist to reinstitute topical corticosteroids for approximately a six week course.
PRK was the first of the corneal laser procedures. It decreased in popularity with the introduction of LASIK, but in the last decade, with topical mitomycin and trans-epithelial techniques, has re-emerged as a safe, accurate and viable corneal laser method, which should be considered as part of a battery of options for patients.
LASER IN SITU KERATOMILEUSIS
Excimer lasers were initially used to perform PRK. LASIK overcame the issues of pain and delayed healing, and expanded the range to include higher myopic corrections. LASIK as a concept was first described by Peyman in 1985.7 Pallikaris, in Greece in 1988, described the creation of a lamellar corneal flap with the microkeratome and then application of the excimer laser to the host’s stromal bed under the flap. It was Pallikaris who coined the term laser in situ keratomileusis (LASIK). The excimer laser was approved by the USA Food and Drug Administration (FDA) in 1995 and LASIK was approved by the FDA in 1999, so there is now a generation which has grown up with the procedure.
Mechanical microkeratomes were used until a femtosecond laser was first developed to create the corneal flap in 2003. In a landmark publication in 2016, Sandoval et al8 examined 97 relevant articles, which represented 67,893 eyes. The aggregate loss of two or more lines of corrected distance visual acuity was 0.61 per cent. The overall percentage of eyes with uncorrected distance visual acuity better than 6/12 was 99.5 per cent. The spherical equivalent refraction was within +/-1.00D of the target refraction in 98.6 per cent of eyes, and 90.9 per cent within +/- 0.50D.
In 2009, the American FDA instituted the LASIK Quality of Life collaboration project. Two major components of this project were the first FDA initiated clinical studies of LASIK – the Patient Reported Outcomes with LASIK (PROWL) studies. PROWL 1 and PROWL 2 were primarily concerned with the development and testing of a validated questionnaire to capture patients’ perceptions of LASIK and the percentage of patients having difficulty after surgery. PROWL 1 was conducted by a single US Navy refractive surgeon and the PROWL 2 trial by five refractive surgeons. Industry and organised ophthalmology were not involved in the study. For this reason, the results of the PROWL 1 and PROWL 2 trials are considered the most definitive evaluation of the efficacy of LASIK. The PROWL studies showed that following LASIK there was a marked improvement in visual symptoms which existed prior to surgery with glasses and contact lenses, particularly regarding ghosting, glare, and haloes. For most patients with visual symptoms, LASIK improves the quality of vision. A minority of patients who are asymptomatic preoperatively developed new symptoms after LASIK.
LASIK is a versatile procedure. It can treat a wide-range of myopia and astigmatism, and also hyperopia and astigmatism. The most feared complication, weakening of the cornea, still occurs but is very rare. Screening of the corneal anatomy preoperatively has led to this reduction in ectasia. It is important to remember that LASIK, like all corneal refractive procedures, will always weaken the cornea. Ectasia can therefore occur if the surgery is performed in an already weak cornea, or more rarely, if too much surgery is done in a normal cornea, so it is excessively thin and pushes it into a weakened state.
SMILE is considered a more surgically demanding procedure… improvements in surgical experience and technique, and adjustments in energy settings, do lead to less complications and faster visual recovery
LASIK does not need to be pushed beyond its limits and as a general rule, a myopic correction of up to 8.00D, an astigmatic correction up to 4.00D, and a hyperopic correction of up to 3.00D would be considered acceptable. Of course this depends on the patient’s expectations, corneal anatomy, tear quality, and age.
As the amount of treatment increases, the accuracy of the procedure decreases, and the ability to perform enhancement is reduced because of the amount of tissue removed. The excimer approach to LASIK can be WaveFront guided, WaveFront optimised, and in more recent years, topography guided. These developments, along with accompanying improvements in ocular registration, have all demonstrated value for improving optical outcomes and expanding the capabilities for treatment customisation.
SMALL INCISION LENTICULE EXTRACTION
Small incision lenticule extraction (SMILE) is the clinical realisation of earlier efforts to create an intrastromal procedure, which can negate the need to create a LASIK flap. The first sighted human studies undergoing intrastromal treatment were published in 2008, by Sekundo et al,9 using the VisuMax femtosecond laser by Carl Zeiss Meditec AG. Since that time over 1,500,000 SMILE procedures have been performed and results are largely comparable to refractive results with LASIK in studies of myopia and myopic astigmatism. By removing the need to create a corneal flap there is reduced disruption of corneal subbasal nerve density and reduced impact on corneal sensation and ocular surface symptoms, such as dry eye. Any procedure offering relative preservation of native corneal nerve morphology and function should be helpful. The second potential advantage with SMILE is that by avoiding a flap it leads to relative preservation of the anterior stromal architecture and its associated biomechanical strength. A number of studies support the theoretical and measured biomechanical advantages of SMILE over flap based procedures such as LASIK. Unfortunately, our knowledge of an individual’s biomechanical makeup is currently limited and this handicaps the surgeon’s ability to recommend the most structurally appropriate procedure. Therefore, the exact place of SMILE, in terms of preserving corneal strength and preventing ectasia, is still being debated by the profession.
Vision is slower to recover with SMILE compared to LASIK. In a head to head study of LASIK vs. SMILE, by Chiche et al,10 LASIK had significantly better contrast sensitivity during the first week, and better patient reported quality of vision at one week. These differences were resolved by one month and patient satisfaction scores were no different for the two procedures at any time point.
SMILE is considered a more surgically demanding procedure than LASIK and improvements in surgical experience and technique, and adjustments in energy settings, do lead to less complications and faster visual recovery.
I consider SMILE the first choice for a patient above -3.00D of myopia, with or without coexisting astigmatism. LASIK is therefore used for smaller amounts of myopia and astigmatism, and for hyperopic treatments. PRK is used generally where the corneal anatomy is not appropriate for either SMILE or LASIK, and sometimes because of patient preference. This requires a conversation with the knowledge that each have their place, and that no one procedure is there at the exclusion of others.
WHAT’S MADE CORNEAL REFRACTIVE SURGERY BETTER IN 2019?
The Availability Of Options
We now have PRK, LASIK and SMILE to choose from. This means we can tailor a treatment with more specificity. If a patient is returning to body contact sport in the first week, then SMILE makes sense. If a patient needs their vision to be as close to normal as possible within 24 hours, then LASIK is appropriate. If they are risk averse or do not have a corneal anatomy suitable for LASIK or SMILE, then PRK is the choice.
Screening For Possible Ectasia
With advances in tomography and an understanding of risk factors for ectasia, the incidence of this serious complication is rare and it is hoped that SMILE may reduce it further. The current position is that any corneal laser procedure will weaken the cornea. If it is weak preoperatively, ectasia is possible. If we do too much in a strong cornea, then that also puts that eye at risk of ectasia. Screening is all about identifying a potentially weak cornea. Respecting the limits for the three procedures is responsible medicine.
Our Understanding of Dry Eye
We now recognise that dry eye is endemic with modern life and digital devices. Recognising it preoperatively with specific tools such as the OSDI questionnaire and tear osmolality, managing it when necessary preoperatively, and excluding those who should not proceed, has made a great difference to the safety and efficacy of corneal refractive surgery.
improved safety and quality of lens removal and IOL surgery has meant patients in their early 50s and 60s have an option other than corneal refractive surgery
Implantable Contact Lenses
The availability and improvement of implantable contact lenses (ICLs) has meant that the limits of corneal refractive surgery do not need to be pushed. The ICL with the centraflow hole has meant that peripheral iridotomies are no longer required prior to ICL surgery, and their accuracy and safety continues to be demonstrated the longer they are followed.
Safety of IOL Surgery
In a similar way to ICLs, the improved safety and quality of lens removal and IOL surgery has meant patients in their early 50s and 60s have an option other than corneal refractive surgery.

Figure 2. A Morcher pinhole secondary IOL in situ
THE JURY IS STILL OUT
Crosslinking, in combination with LASIK, may be a relevant technique. The essential issue is that for crosslinking to be effective, it has to affect the cornea in a way that impinges on corneal clarity and refractive outcome. Combining it with LASIK means we are potentially decreasing the accuracy of an extremely accurate procedure. LASIK can be performed in conjunction with a small amount of crosslinking, but it may mean that the crosslinking is not effective. The dilemma is that it will take many years to know whether this has an impact on ectasia. With more targeted crosslinking, which is sure to be available in future years, I think this issue will be revisited and may have some merit.
WHAT DIDN’T WORK BUT LED ELSEWHERE?

Figure 3. Eyebanks are considering ways to recycle SMILE lenticules
Corneal Inlays
In their various forms they have come and gone as expected. A corneal inlay alters the shape of the cornea too much and for the few successes, there were too many unhappy patients with irregular astigmatism and dry eye, and just not reading well enough to make these viable procedures. What has happened with the Kamra inlay is that the inlay has gone inside the eye. This is a much better idea. The IC8 is a forgiving lens. This lens is used in conjunction with normal cataract and is helpful in a post refractive eye if you are worried about getting the power right. It is also useful in the nondominant eye as mini monovision without having to induce excessive myopia. The Morcher pinhole secondary intraocular lens is used when there is already an intraocular lens in place, and this has a more specific role in overcoming significant corneal aberrations, where a corneal transplant needs to be avoided. A poor idea in the cornea has led to a good idea inside the eye.
Don’t Be Distracted By . . .
The claims regarding various ways of performing LASIK. Conventional LASIK always induced spherical aberrations. For this reason, alternatives were sought; WaveFront guided and WaveFront optimised. There is no discernible difference in large studies and they both work well. The aim is not to increase preexisting higher order aberrations (HOAs). Occasionally it is helpful to perform WaveFront guided LASIK in a patient with a large HOA profile preoperatively, but these are rare patients. More recently, topography guided LASIK has been available and it is a good procedure. However, despite being exceptionally good in a small series, it is unlikely to be any better, or worse, than WaveFront guided or optimised. So don’t be distracted – all of these LASIK procedures are excellent.
Presbyopic LASIK
This aims, in a variety of ways, to alter the corneal shape to improve near vision without having to induce so much myopia. The problem is presbyopic LASIK relies on increasing spherical aberration and increasing the depth of focus, or producing a multifocal effect. This is a poor option in terms of visual quality. When applied in a very mild form, it probably does improve the range of vision subtly but not in a meaningful way. So don’t be distracted by presbyopic LASIK. Presbyopia will always be dealt with inside the eye.
WATCH THIS SPACE
Recycling
In a world of recycling, it seems a waste to throw away a perfectly good corneal SMILE lenticule. So don’t! Eye banks around the world are looking at harvesting this material and using it in a variety of ways such as strengthening procedures in keratoconus, helping with hyperopic LASIK or hyperopic SMILE, and in ways that are still yet to be established. A procedure to deal with myopia and astigmatism will end up providing tissue to biobanks, which can be used for other purposes.

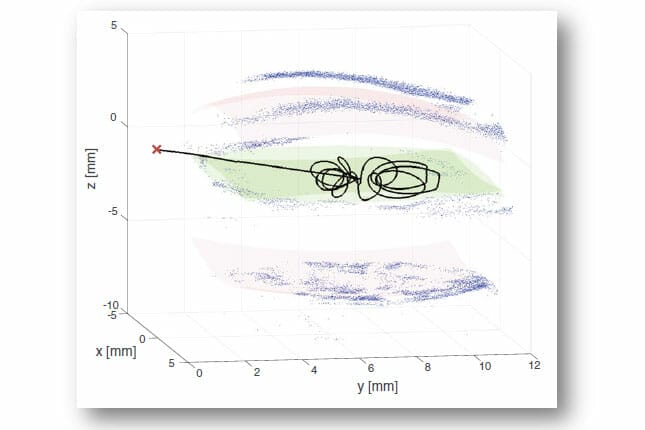
Figure 4. IRISS trajectory
Robots
The robots are coming. The first real robotic eye surgery was performed in 2015 (a robotically-assisted pterygium surgery). The team never did another procedure as it was too cumbersome and slow. The feeling always was that robotic surgery will have a place in retinal surgery and in procedures where the steadiness of a robot can enhance the human surgeon with spatial resolution and the delineation of layers, or perhaps the cannulation of small vessels. We also felt that robots would not be able to perform cataract surgery given the multiple manoeuvres in a 3D space. Well that view is changing. In 2018, Chen et al,11 published on their intraocular robotic interventional surgical system (IRISS). Their initial report on 30 pig eyes showed 25 lens removals performed purely by the robotic system without incidence. So the robots are coming, but maybe not for a few years yet.
Big Pharma
If the robots won’t get you, then ‘big pharma’ might. UNR844L is the presbyopia magic drop. It is a lipoic acid choline ester. The theory is that progressive stiffening of the lens occurs because of oxidation of adjacent lens proteins and that this drop may reduce restricting covalent bonds between adjacent proteins and allow an increase in the amplitude of accommodation. Use of this topical medication may delay presbyopia, and indeed, may delay nuclear sclerosis cataract. In trials over three months, the drop has not been associated with adverse events and appears to be moderately effective.
In a world of recycling, it seems a waste to throw away a perfectly good corneal SMILE lenticule. So don’t!
The start up Encore Vision was acquired by Novartis in early 2017 and every adult in the world above the age of 40 will be watching the development of this medication with great interest.
Clinical Associate Professor Michael Lawless was one of the first ophthalmic surgeons in the world and the first surgeon in the Southern Hemisphere to perform femtosecond laser for cataract surgery. His areas of specialisation are laser vision correction, cataract surgery, lens surgery, refractive lens exchange, and corneal transplants.
References
- Trokel SL, Sirnavasan R, Braren, B. Excimer laser surgery of the cornea. American Journal of Ophthalmology 1983: 96; 101-715
- Lawless M, Chan C, Hodge C, Sutton G. Tear osmolarity in 1150 consecutive patients attending for vision correction surgery. Oral presentation, RANZCO annual congress, November 2018.
- Barsam A, Allan BDS. Excimer laser refractive surgery versus phakic intraocular lenses for the correction of moderate to high myopia. Cochrane Database of Systematic Reviews 2014, Issue 6. Art. No.: CD007679. DOI: 10.1002/14651858.CD007679.pub4.
- Mehlan J, Linke SJ, Skevas C, et al. Safety and complications after three different surface ablation techniques with Mitomycin C: a retrospective analysis of 2757 eyes in 2018. Graefes Arch Clin Exp Ophthalmol 2018 Aug 3. doi: 10.1007/ s00417-018-4077-7 [Epub ahead of print]
- Majmudar PA, Schallhorn SC, Cason JB, et al. Mitomycin C in corneal surface excimer laser ablation techniques: a report by the American Academy of Ophthalmology. Ophthalmology 2015 Jun;122(6):1085-95
- Sutton G, Lawless M. “Looking beneath the surface”. Clin Exp Ophthalmol. 2014 May-Jun;42(4):309-10
- Lawless M, Hodge C. LASIK. Int Ophthalmol Clin. 2013 Winter;53(1):111-28
- Sandoval HP, Donnenfeld ED, Kohnen T, et al. Modern outcomes with LASIK. J Cataract Refract Surg. 2016 Aug;42(8):1224-34
- Sekundo W, Kunert K, Russmann C, et al. First efficacy and safety study of femtosecond lenticule extraction for the correction of myopia: six-month results. J Cataract Refract Surg 2008; 34:1513–1520
- Chiche A, Trinh L, Saada O, et al. Early recovery of quality of vision and optical performance after refractive surgery: Small-incision lenticule extraction versus laser in situ keratomileusis. J Cataract Refract Surg. 2018 Sep;44(9):1073-1079
- Chen CW, Lee YH, Gerber MJ, et al. Intraoperative robotic interventional surgical system (IRISS): Semi automated OCT guided cataract surgery removal. Int J Med Robot. 2018 Dec;14(6):e1949. doi: 10.1002/rcs.1949









